Looking after your wound
Looking after your wound
This information is for patients being cared for by our District Nursing and/or Tissue Viability teams. It explains how to look after your wound, how to recognise signs of infection and when to ask for help. It also explains about your wound care appointment.
What is a wound?
Your skin is made up of many different layers. A wound is an injury that breaks the skin or damages underlying biological tissues such as muscles, bones or organs.
Wounds may have a variety of causes, such as accidents or surgery, or can occur as a result of frail skin or being bed bound. Wounds may be called different things depending which layer of skin they are in.
For example, if the damage to your skin is in the upper layers, it may be called a graze, a skin tear, or a blister. If the damage in your skin goes deeper into the lower layers, it may be called a wound or an ulcer.
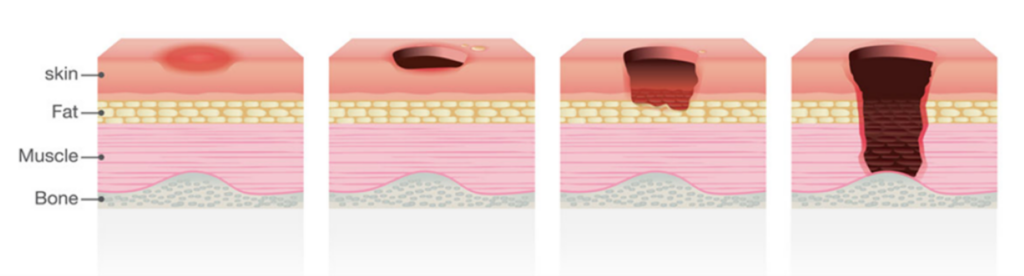
All breaks in your skin can cause you problems, but damage to the deeper layers may cause you more damage and take longer to heal.
If you have been referred to our District Nursing and/or Tissue Viability service it is usually because you have a complex wound that requires the support of a healthcare professional to assist the healing process.
Looking after your wound
To give your body the best chance to fight infection and heal your wound, it’s important to take care of yourself and your wound.
Wounds may heal more slowly if you smoke, have a health condition such as diabetes or rheumatoid arthritis or are on medication that helps you in other ways but may slow healing.
Here are some simple things that will help the healing process:
- Rest – try to rest, sleep well and look at ways to reduce the stress in your life.
- Eating healthily – this will help the healing process; you may need to increase the amount of protein you eat because your body needs protein to help mend your body. This is particularly true if you have multiple wounds, or your wounds are weeping fluid. Try to have a protein source at each meal and include high protein snacks between meals.
- Keeping your wound dry – it’s important to keep your wound/dressing as dry as possible, so you may need to change your bathing routine. If possible, have showers rather than baths so that your wound does not soak in water. Only have a bath if you can keep your wound out of the water.
Checking for infection
It’s important to check your wound regularly for infection. Signs of infection can include:
- redness around the wound
- skin around the wound feeling warmer than normal
- increasing pain in or around the wound
- swelling or hardening of the surrounding skin
- increased fluid or leakage from the wound
- an offensive smell
- yellow or green pus
- the wound becoming larger or deeper.
What to do if you think your wound is infected
If you notice any of the above signs and are worried about your wound, please call the Duty Nurse at any time on 01274 221221.
If redness is spreading across a larger area of skin, this may mean the infection is spreading. In this case contact your GP practice, or contact NHS 111 online at https://111.nhs.uk or by calling 111.
-
Your nurse will agree a wound care plan with you – please ensure you keep that information safe.
Your plan may include:
- how your wound and surrounding skin should be cleaned
- which dressing to use (including bandages, wraps or hosiery if needed)
- how often the dressing should be changed
- any additional advice to help your wound heal.
If you have any concerns before your next review, please call us on 01274 221221.
-
If your nurse has shown you how and provided the correct supplies you can change your dressing safely at home by following the guidance below. This may be useful if you are unable to attend clinic every time your dressing needs changing. It’s helpful to read this through completely before you get started.
What you need to change your dressing
You will need a clean, flat surface such as a table or kitchen work surface to put the new dressings on. Before you start, clean the surface using sanitising wipes, or a solution of warm water and washing up liquid.
Your nursing team will provide everything else you need, including:
- a dressing pack (gloves, gauze, tray, apron and waste bag)
- the wound dressing recommended for you
- disposable scissors (if needed)
- creams or barrier creams (if part of your care plan – important: a build up of cream on clothes, bedding or furniture can cause a fire hazard, please see our skin care safety advice)
- wound cleansing solutions (if advised by your healthcare professional).
Washing your hands
Hand hygiene is extremely important. Always wash your hands thoroughly before and after touching your wound or dressing.
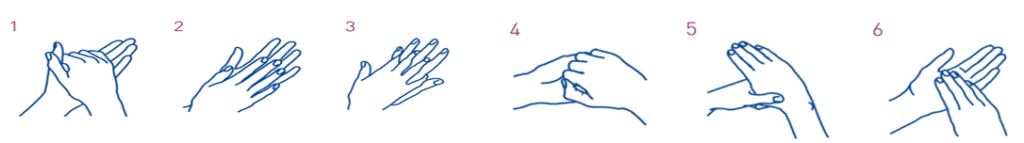
Spend 20 seconds washing your hands, paying special attention between your fingers and on the palms of your hands. Dry your hands with a clean towel or kitchen paper.
Gather what you will need
Place everything you need to change your dressing on the surface you have cleaned so it’s in easy reach.
Step-by-step guide to changing your dressing
- Place the dressing pack on your firm, flat, clean surface.
- Open the dressing pack carefully by peeling the edges. Do not touch the inside of the pack.
- Put on the apron provided.
- Use the waste bag to create a sterile glove on one hand.
- Using the bagged hand, lay out all items from the dressing pack on the clean surface.
- Open the new dressings by peeling the packaging open. Do not touch the inside. Place them on the clean surface.
- Remove the old dressing carefully. Do not touch the inside of the dirty dressing or the wound. If the dressing is stuck, do not pull. Wet it with tap water and gently remove it.
- Put the old dressing and packaging into the waste bag.
- Wash your hands again.
- Put on the clean gloves from the pack.
- Fill the tray with clean, warm tap water.
- Clean the wound and surrounding skin using soaked gauze.
- Dry the area with clean, dry gauze.
- Apply the new dressing as advised by your nurse.
Unsure what dressing to use?
Only use the dressing recommended by your nurse. If you are unsure or have run out of supplies, contact your nursing team for advice on 01274 221221.
What should I do if my wound looks worse?
If you notice increased redness, pain, swelling, discharge, or a bad smell, please contact us on 01274 221221.
If redness is spreading over a larger area of skin, contact your GP practice or NHS 111 online at https://111.nhs.uk or by calling 111.
-
Why have I been offered a clinic appointment?
You will be offered a clinic appointment if your District Nursing team has assessed your needs and, using NHS criteria, you are not classed as housebound.
Community nurses visit people at home when they cannot safely leave home. For you, clinic care is the safest and quickest way to help.
Care in a clinic can be better than care at home because clinics have specialist equipment that keeps you and our staff safe and comfortable, reducing the risk of injury.
You can book clinic appointments to fit around your needs at a time that is convenient for you.
What help can I get to attend?
Tell us what would make it easier. We can offer reasonable adjustments, for example:
- a longer or quieter appointment time
- an accessible room and nearby parking
- having a carer or friend with you
- information in large print or another language
- an interpreter or BSL support, or
- waiting in your car until we call you in.
If you need any other adjustments, please let us know when booking.
Getting to your appointment
If you are unable to drive, family or friends may be able to help. Taxis, private cars, mobility scooters, the bus, or access bus may also be options
If you have a Blue Badge, please bring it so you can make use of appropriate parking spaces.
How can I get the most out of my appointment?
Please try to arrive in good time for your appointment. If you arrive late, it may not be possible to see you.
If you are unable to attend your appointment please let us know so we can arrange a different time for you to come to clinic – call us on 01274 221221.
If you do not attend your appointment and do not let us know that you will not be coming, we will try to contact you by telephone to arrange a different appointment time. If we cannot contact you, and you do not telephone us within a week of not attending, you will be discharged from the service.
What if I’m still worried about attending?
Please tell us. We’ll work with you to find a plan.
If your health worsens (for example: fever, severe pain, shortness of breath), contact your GP, NHS 111, or 999 in an emergency.Your assessment and adjustments
We record the assessment and any adjustments agreed. If you decline a clinic appointment, we note this and provide you with safety advice.
How can I give feedback or challenge the decision?
You can contact our Patient Advice and Complaints team by phone on 01274 251440 or by email at advice.complaints@bdct.nhs.uk